|
Back to Blog
2 1 atrial flutter5/21/2023  With an ageing population, it is becoming increasingly common. Around 50% of those presenting with atrial flutter alone are said to develop atrial fibrillation within the next eight years. 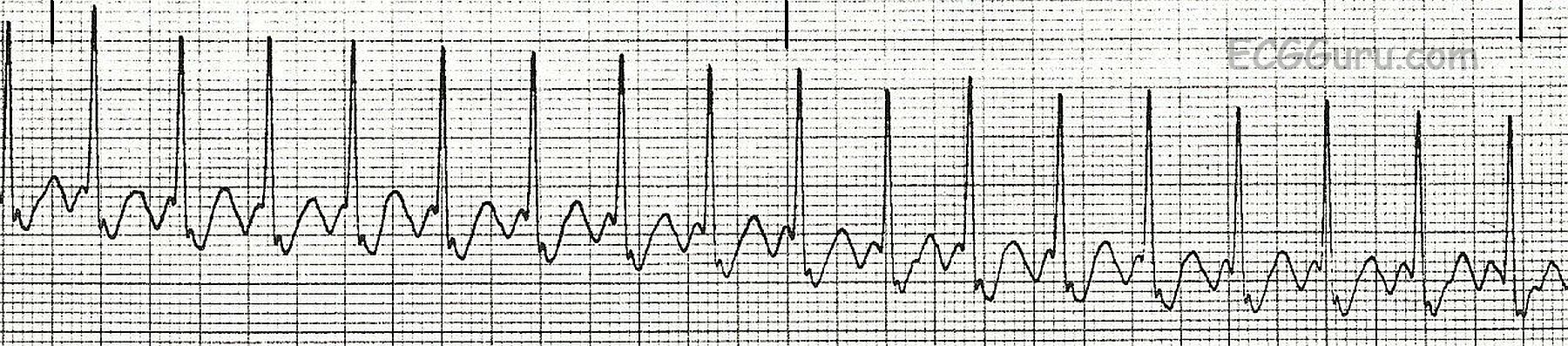
Atrial flutter is commonly associated with atrial fibrillation.It is the second most common arrhythmia after atrial fibrillation.It is one tenth as common as atrial fibrillation. Atrial flutter is less common than atrial fibrillation, but epidemiology is less well studied.ECG patterns are variable and there may be faster atrial rates than in typical flutter. This is also called non-cavotricuspid isthmus-dependent atrial flutter. In atypical atrial flutter, the origin is elsewhere in the right atrium or the left atrium.The ECG pattern shows regular mainly negative atrial deflections in the inferior leads with a 'saw-tooth pattern' at rates of 240-350 bpm per minute. 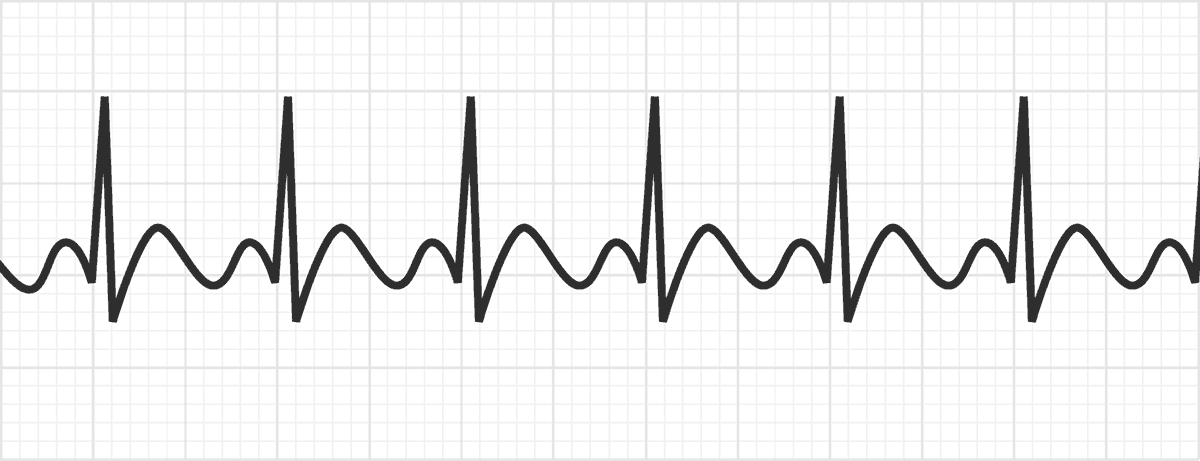
This is also called cavotricuspid isthmus (CTI) or common atrial flutter. In typical atrial flutter the rhythm has its origin in the right atrium at the level of the tricuspid valve.Like atrial fibrillation, it can be paroxysmal or persistent. Atrial flutter is a macro-reentrant tachycardia and can be classed as typical or atypical atrial flutter depending upon the origin. There is typically an atrial rate of around 300 beats per minute (bpm) and a ventricular rate that may be fixed or be variable. 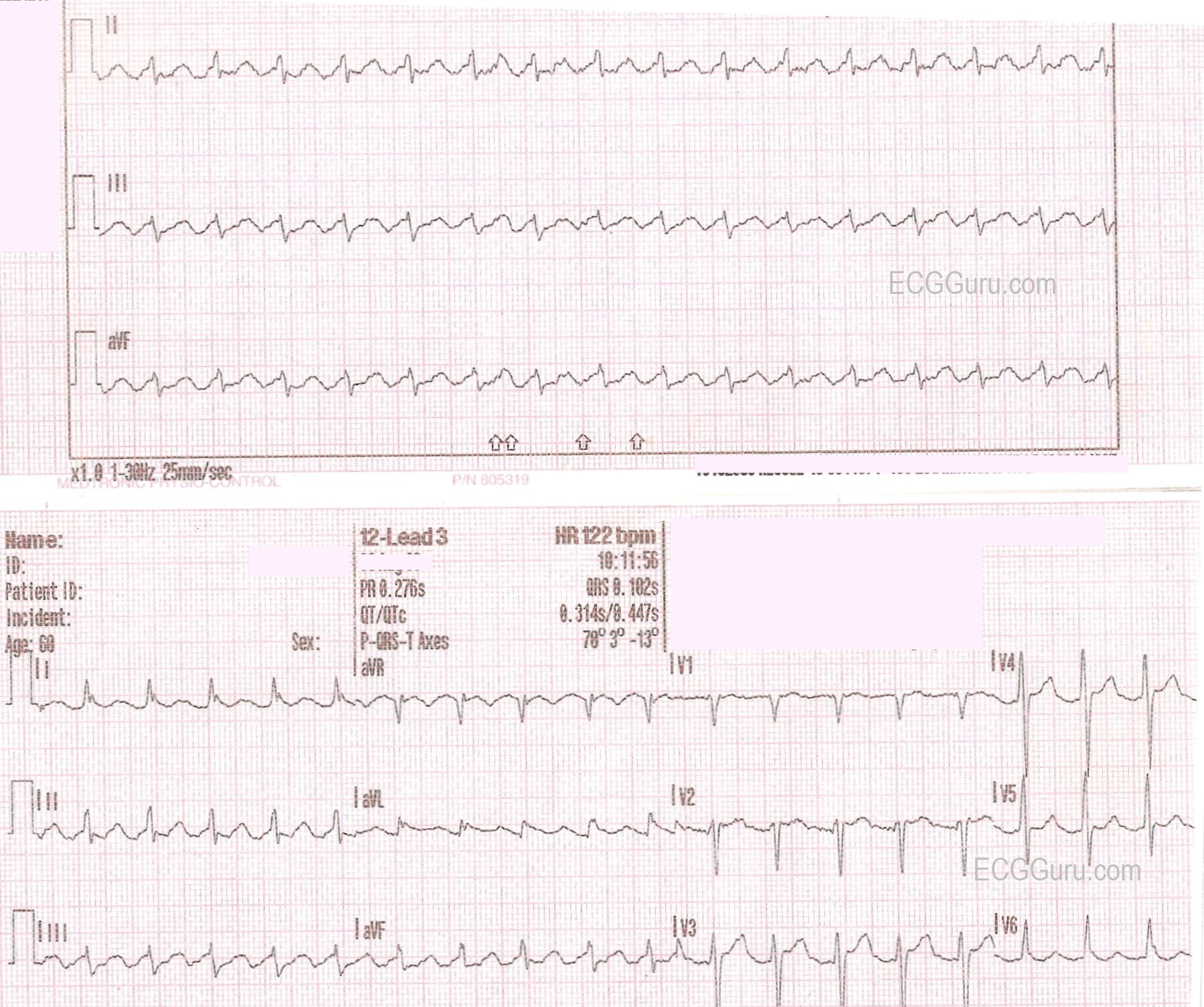
Pathophysiology Ītrial flutter is characterised by an abnormal and rapid heart rhythm. See also the separate Atrial Fibrillation article. Both arrhythmias can cause clinical symptoms such as palpitations, syncope and fatigue, and are associated with a risk of thrombus formation and thromboembolism. European and American guidelines cover the conditions separately although there, much of the management is the same. There are many similarities in clinical presentation and management, and indeed the guideline from the National Institute for Health and Care Excellence (NICE) makes hardly a distinction, stating the guideline for atrial fibrillation applies to patients with atrial flutter, specifying a particular management in the latter only in one sentence. Many patients with atrial flutter have associated atrial fibrillation. If this happens, the procedure may be repeated or you and your health care provider might consider other treatments.Atrial flutter is one of the more common atrial arrhythmias (supraventricular arrhythmias). Most people see improvements in their quality of life after this type of cardiac ablation, but there's a chance the atrial flutter may return. ResultsĪfter atrial flutter ablation, you'll need regular checkups to monitor your heart. Afterward, you'll be taken to a recovery area where care providers will closely monitor your condition.ĭepending on your condition, you may be allowed to go home the same day or you may spend a night in the hospital. The scarring helps block the electrical signals that are causing the atrial flutter.Ītrial flutter ablation typically takes two to three hours. Heat (radiofrequency energy) is applied to the target area, damaging the tissue and causing scarring. This information is used to determine the best place to apply the ablation treatment. Sensors on the tip of the catheter send electrical impulses and record the heart's electricity. The doctor inserts a long flexible tube (catheter) into the vein and carefully guides it into your heart. Once the sedative takes effect, a small area near a vein, usually in your groin, is numbed. You'll likely receive a medication to help you relax (sedative). What you can expectĪtrial flutter ablation is done in the hospital. Atrial flutter ablation may restore a typical heart rhythm, which may improve quality of life. Atrial flutter ablation is done to control the signs and symptoms associated with atrial flutter. 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
